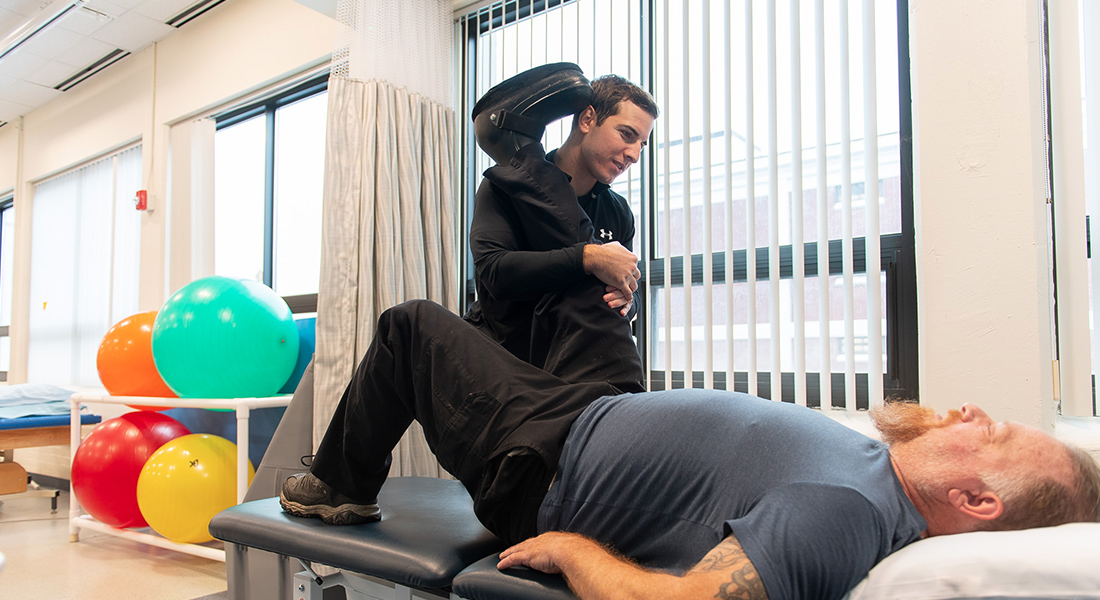
Rehabilitation Programs & Services at Salem
With a combination of highly trained people and the most advanced rehabilitation treatments and research available, we’re here to support you and your family through a variety of therapy needs.
- Physical Therapy
- Hand Therapy
- Neurological Rehabilitation
- Occupational Therapy
- Physical Medicine and Rehabilitation (PM&R)
- Speech & Language Pathology/Voice Therapy
- Spine Care
- Pelvic Health Rehabilitation
View our full list of services
Meet the Team

Standouts in the Field. And in Your Corner
Our team, considered among the best rehabilitation clinicians and therapists in the field, are ready to help you be your best.